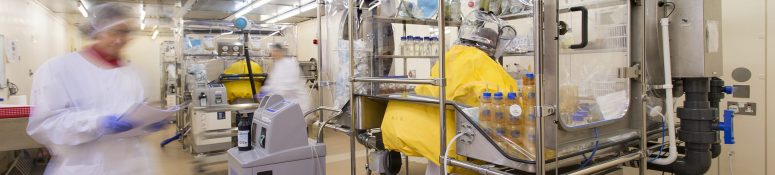
Animal-Free Bacterial Endotoxin Testing
The Recombinant Reagents
Type:
Published:
Author:
Cormica Microbiology Department
Request call back

Following on from our previous article, we wanted to summarise the journey to animal-free bacterial endotoxin testing with an overview of the recombinant reagents. As it stands, there are two commercially available recombinant reagents: Recombinant Factor C (rFC) and Recombinant Cascade Reagent (rCR).
Before we discuss each in turn, we would like to emphasise a key feature of both recombinant reagents: they are endotoxin-specific. This means that both types of recombinant reagents will only be activated when in the presence of endotoxins. Limulus Amoebocyte Lysate (LAL) reagents on the other hand, will become activated by both bacterial endotoxins as well as fungal 1,3-beta-glucans via the Factor G pathway. This is an innate immune response of the Horseshoe Crab (HSC) in the presence of bacteria and fungi.
This additional pathway poses a challenge when it comes to testing samples that contain beta-glucans, as it can cause a synergistic reaction with the Factor C pathway for endotoxins. Not only can this lead to an invalid method suitability (often seen as spike recoveries above 200%) but in more extreme cases the reported results may exceed the endotoxin specifications, thus triggering out of specification (OOS) investigations. Troubleshooting the testing issues and leading OOS investigations caused by beta-glucans can be costly in terms of time and resources.
While there are buffers available that can inhibit the Factor G pathway, their efficacy in eliminating the synergistic relationship may be influenced by the type and amount of the beta-glucans present. However, because the recombinant reagents are synthetic, Factor G is not included in either rFC or rCR. While this may seem like a minor point, the resulting endotoxin specificity that the recombinant reagents inherently provide, allows for an increase in specificity, accuracy, reproducibility and repeatability of the assay in samples containing endotoxins (Marius et al, 2017).
Another exciting feature of both recombinant reagents is their lot-to-lot consistency. As LAL reagents consist of a complex mix of enzymatically active proteins – including but not limited to Factor C, Factor B, Pro-clotting enzyme, Coagulogen, and Factor G – the final enzymatic activity is highly likely to vary between lots, even when the assay is well-developed and well-controlled. However, recombinant technology allows for a higher degree of control and characterisation of the peptides within different steps of the manufacturing process, thus leading to a documented degree of lot-to-lot reproducibility when compared to the compendial LAL reagents (Muroi et al, 2019).
Recombinant Factor C (rFC): A Pioneering Alternative
Having been commercially available since 2003, rFC was the first recombinant reagent for bacterial endotoxin testing. By expressing the DNA for Factor C in cell lines, manufacturers were able to effectively develop an animal-free reagent as an alternative to the animal-based LAL reagents for a bacterial endotoxin test (BET). As this was the first of its kind, there are some differences to the LAL photometric reagents most commonly used today.
Firstly, as rFC is based on the work of Dr. Jeak Ling Ding, who conducted her initial research in Singapore, it uses the genetic material of the Carcinoscorpius species of HSC that is local to that region (Ding et al, 1995). This means that rFC is based on the Carcinoscorpius Amoebocyte Lysate cascade (CAL) as opposed to the LAL cascade.
While Factor C is a critical component of the endotoxin reaction (acting as the sole biosensor for bacterial endotoxins), the other two factors are responsible for the amplification of the signal, so their absence means that the limit of quantitation of rFC reagents would be insufficient to meet the endotoxin specifications for even the most commonly tested sample: Water for Injection (endotoxin limit < 0.25 EU/mL). To mitigate this, the signal of activated rFC is amplified chemically through the use of a fluorescent assay, which allows it to be read using a fluorescence microplate reader.
The other notable difference between LAL and rFC is the test set up and data interpretation. When performing a kinetic BET, there is a single reconstitution step when reconstituting the reagent. With rFC, there are three reagents that must be reconstituted in a certain ratio, as well as a 10 minute pre-incubation step. This, along with the fact that rFC can only be performed as an end-point assay as opposed to a kinetic assay, makes performing the rFC test markedly different to performing the LAL test.
Recombinant Cascade Reagent (rCR): Next-Generation Evolution
The first generation of recombinant cascade reagents was based on the genome of Tachypleus tridentatus, so used the three factors from the Tachypleus Amoebocyte Lysate (TAL) cascade. Having been commercially available in Japan since 2015, this reagent was further developed into a recombinant cascade reagent based on the genome of Limulus polyphemus, which was released in 2021 as the next generation reagent.
The key difference between rFC and rCR is that rCR consists of all three factors of the LAL cascade as opposed to just Factor C. In doing so, rCR utilises the natural amplification mechanism of LAL, which means the signal generated by endotoxins is high enough to be detected using an absorbance reader (Mizumura et al, 2017). There is no need to chemically amplify the signal using fluorescence.
This provides rCR with a key advantage in a QC laboratory setting, in that it can be used with the same instrumentation and method as the LAL test that technicians are used to. When it comes to the mass adoption of animal-free bacterial endotoxin testing, this is a significant step in removing the barriers pharmaceutical and medical device companies face when they look to make the switch.
Another interesting point about rCR is that it was documented to be suitable for a wide range of finished drug products, and in fact may present an advantage in a lower level of interference between the sample matrix and the reagent. This can translate to a lowered Non Interfering Dilution for some samples with rCR when compared to rFC or LAL (Stevens et al, 2022). For example, when testing a Sodium Citrate injection for transfusion (potency of 100 mg/mL) using an LAL reagent, you may need to dilute that sample to 1:4 or higher to overcome product-specific interference. However, when using rCR on the same sample, the injection may not have to be diluted (1:1).
While this might seem like an insignificant feature when comparing LAL with rCR on paper, this makes a huge difference when using this reagent in a QC laboratory environment. Aside from the cumulative time savings gained by removing a dilution step, this may even allow laboratories to test a product they were previously unable to test using LAL, as the dilution required to overcome any interference may have been above the Maximum Valid Dilution for that product.
Conclusion and Cormica’s Commitment
While rFC does have some key differences to the LAL kinetic methods, this does not change the fact that it is an effective animal-free solution to bacterial endotoxin testing. However, it may be partly why there was no dramatic shift away from LAL to rFC when it was released back in 2003. There is no doubt that the complex regulatory environment and the initial lack of comparability data were two major roadblocks preventing its widespread early adoption, but as with most new technologies, it was ultimately overhead cost that was the deciding factor.
As a result of the amount of testing required to perform an alternative method validation and demonstrate that rFC is comparable to LAL on a product-specific basis, the cost for pharmaceutical and medical device companies to use rFC to routinely test their finished products compliantly was significant. When you then consider the additional cost required to purchase fluorescence plate readers and train technicians in a brand new method, it is not surprising that the use of rFC has been confined to the major pharmaceutical companies only.
Although this alternative method validation would also be required if using rCR, the similarity of rCR with LAL does mean that there would be one less obstacle to make the switch. As QC labs routinely performing the LAL test would already have the required instrumentation, and their technicians would already be trained on what is a like-to-like method, there would be no initial capital outlay required to start testing with an animal-free method when using rCR.
While this is an exciting time for the industry, we will close on a warning. As both types of recombinant reagents are no longer biological products, their manufacture is not likely to be regulated by the FDA moving forward. This is an important point, as it is now the case that the manufacture of recombinant reagents is no longer confined to those companies that have a license issued by the FDA, and are therefore maintaining the highest of quality standards. This, along with the fact that recombinant technologies are becoming more accessible, means it is just a matter of time before other recombinant reagents will become available, that may not have been manufactured in the rigorously controlled environment that LAL has been for the past 45 years.
This is no concern to us at Cormica – as we are working with a supplier with a significant track record of quality, experience and GMP manufacture – but it is a critical consideration for those companies looking to bring animal-free testing in to their own QC laboratory. When considering recombinant reagents, it is crucial that companies choose a supplier that not only manufactures their reagent under GMP conditions, but there should also be significant peer-reviewed data available demonstrating that the recombinant reagent in question is comparable to LAL.
Should you have any questions about making the switch to animal-free endotoxin testing, please do not hesitate to reach out to us at sales@cormica.com.
Bibliography
Ding, J. L., Chai, C., Ho, B., & Roopashree, S. D. (1995). Expression of Carcinoscorpius rotundicauda factor C cDNA. Biochem Mol Bio Int, 841 – 9.
Marius, M., Vacher, F., & Bonnevay, T. (2020). Comparison of bacterial endotoxin testing methods in purified pharmaceutical water matrices. Elsevier, 49 – 55.
Mizumura, H., Ogura, N., Aketagawa, J., Aizawa, M., Kobayashi, Y., Kawabata, S., & Oda, T. (2017). Genetic engineering approach to develop next-generation reagents for endotoxin quantification. Innate Immun, 136 – 146.
Muroi, M., Ogura, N., Mizumura, H., Aketagawa, J., Oda, T., & Tanamoto, K. (2019). Application of a Recombinant Three-Factor Chromogenic Reagent, PyroSmart, for Bacterial Endotoxins Test Filed in the Pharmacopeias. Biol Pharm Bull, 2024 – 2037.
Stevens, I., Ogura, N., Kelley, M., D’Ordine, R. L., Mizumura, H., Oda, T., Jahngen, E. G. (2022). Advanced Recombinant Cascade Reagent PyroSmart NextGen® for Bacterial Endotoxins Test as Described in the Pharmacopeias. BPB Reports, 105 – 114.
Related resources
Contact Us
Ready to take the next step? We’d love to hear from you. Contact us today to discuss your testing needs and find out how Cormica can help you achieve your goals.